Elementary school teacher, Andel Hoke suffered from lower back pain that was so excruciating that she couldn’t sit at her desk. Many unsuccessful attempts to diagnose the source of her pain left her with no options and little hope. Hoke tried daily to keep a positive attitude for her students. Once she left the classroom each day she began to isolate herself from family and friends. “I couldn’t be my upbeat self,” she explains. The pain became so great that she was no longer able to participate in any activities with her students. When standing or lying down became her only options, she was losing her love of life. As Andel explains, “I didn’t want to bring the people I care about into my pain.”

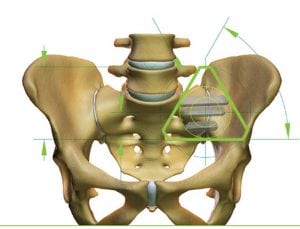
That all changed when she met Dr. Andrew Manista at Olympia Orthopaedic Associates. After hearing Andel’s story, Dr. Manista believed that she was suffering from Sacroiliac Joint Dysfunction. The sacroiliac joint, also known as the SI joint, is located between the sacrum and the pelvis. The SI joint provides support and stability and plays a major role in reducing the impact of daily activities. There are two IS joints located on either side of the body. They are an important shock absorber to prevent the impact of walking from reaching the spine. Hoke could not put any pressure on her spine without feeling incredible pain.
Many patients being treated for spine or hip problems are actually suffering from SI joint pain. For many years this “forgotten joint” wasn’t even a consideration when diagnosing lower back pain. The pain often starts for women during pregnancy when the sacroiliac ligaments are loosened for childbirth. Patients who have undergone spine surgeries can develop problems post-surgery with their SI joint as well.
In the past, the access point to the joint was so difficult and the surgery so “brutal” for the patient that it was rarely thought to be a reasonable treatment option. Dr. Manista admits he wasn’t taught very much about this joint in medical school. However, this changed seven years ago when the iFuse Implant System was introduced. Using the same technology used when repairing a fractured pelvis, the implant allows orthopedic surgeons to access the SI joint through a small incision.
“15-20% of patients with what we call ‘failed back syndrome’ are actually suffering from SI joint dysfunction,” explains Dr. Manista. “This surgery is such a breakthrough for patients who have been suffering from undiagnosed lower back pain.”
Dr. Manista further explains, “Only 10% of those patients will need surgery.” Once the sacroiliac disease is diagnosed, many patients experience much less pain with physical therapy and proper pain management. “Finding out what is causing the pain is paramount,” says Dr. Manista.
After giving Andel an injection directly into the SI joint, Dr. Manista was able to pinpoint the cause of her pain. “I literally melted on the table,” she says. The pain was gone and Dr. Manista knew that he had found the source of her agony. The injection lasted about three weeks. During the pain-free interim, Andel was able to go to a movie and sit for the entire feature, something she hadn’t done in years. Andel was the ideal surgical candidate.
The iFuse Implant System is a breakthrough treatment. The patented, triangular implant is designed to handle the stress of the sacrum, legs and spine all joining in one place. The titanium implant is coated with a patented plasma spray. The porous surface is designed to “grab” bone as it passes by. Bone will grow around the implant over time as the body heals and will strengthen the joint.

Dr. Manista trains other surgeons from around the country on how to diagnose sacroiliac joint pain and implement the iFuse Implant System. Over 20,000 surgeries have been performed with the iFuse Implant System with a 90% success rate. Fortunately, surgery is not the only option. Olympia Orthopaedics Associates has many non-surgical in-house options and works with partners throughout the community. Cortisone injections, physical therapy and sacroiliac belts are all potential treatment options.
Dr. Manista performed the SI implant surgery on Andel Hoke on a Friday morning and she was walking within an hour. “Today I can get on the floor and play with my students,” she says. “My whole outlook on life has changed now that I am pain-free.”
Drs. Douglas Taylor and Andrew Manista will be providing an educational seminar on Sacroiliac Joint Pain at their Westside clinic on Thursday, February 16 from 6:00 – 7:00 p.m. For more information or to RSVP, please contact Rachel Sherburne at 360-570-4862.